Published: 11/17/2023
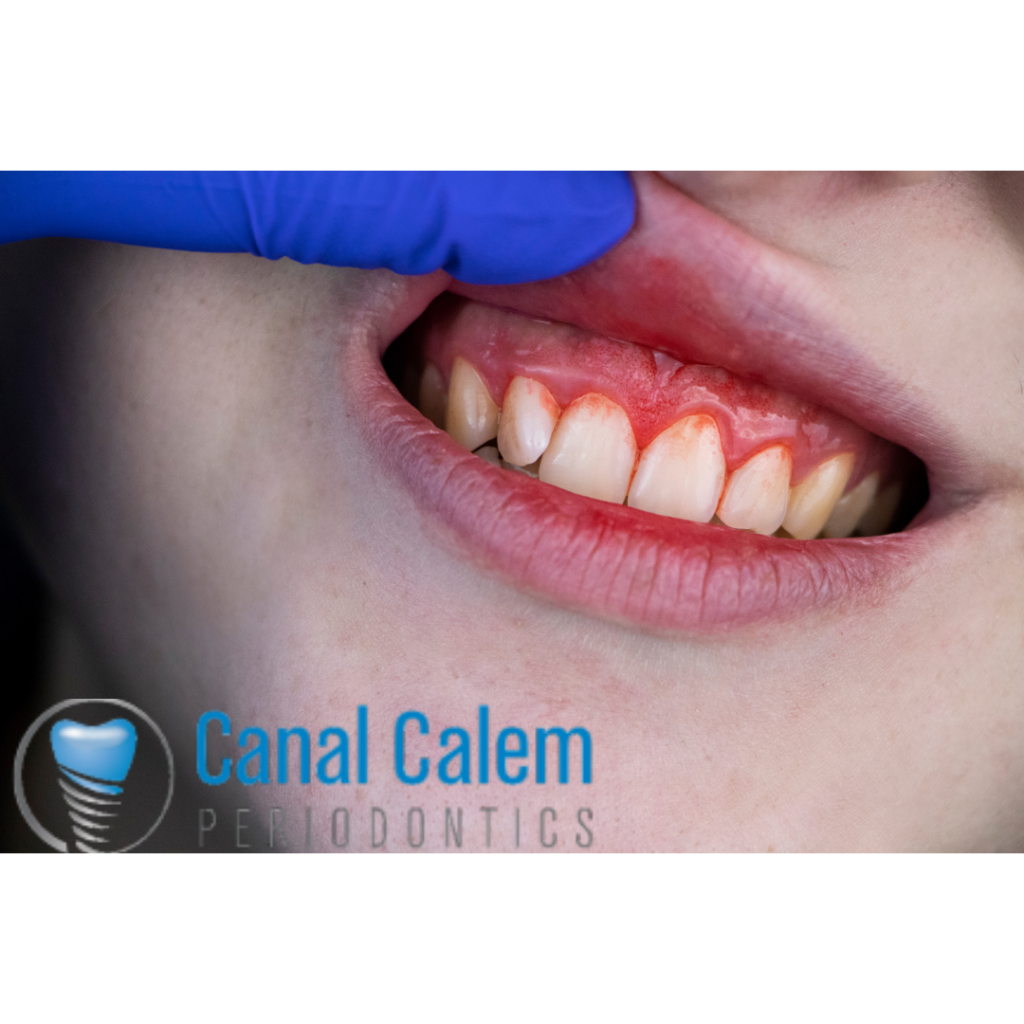
Is no more bleeding the same as no more symptoms?
The moment you notice that your gums have stopped bleeding can be a profound relief. For many, it signals the end of a worrying problem and is often taken as a sign of restored oral health. However, this cessation of bleeding might not be the all-clear signal for gum disease that one might hope for.
Bleeding is a common symptom of gingivitis, the earliest stage of gum disease, and its resolution may lead to the assumption that the gums have healed. But periodontal issues can lurk beneath the surface, often without any noticeable discomfort. This blog post aims to delve deeper into the narrative of gum disease, dissecting the truth behind bleeding gums and their cessation. Our goal is to inform those with preliminary dental knowledge about the intricacies of gum health, illustrating that the journey to optimal oral wellness may extend beyond the absence of bleeding.
Join us as we explore the silent progression of gum disease and why a symptom-free mouth isn’t always synonymous with disease-free gums. For those who are proactive about their dental health, this read is not just an eye-opener but a guide to better understanding and managing one’s oral care routine.
Understanding Gum Disease
Gum disease, known in its various stages as gingivitis to advanced periodontitis, is a progressive condition that affects the tissues supporting the teeth. Periodontitis is the more severe form that follows untreated gingivitis, which begins as a simple inflammation of the gums caused by the accumulation of plaque—a sticky film of bacteria.
The Stages of Gum Disease: From Gingivitis to Advanced Periodontitis
Gingivitis is the earliest stage, where the gums might be red, swollen, and bleed easily. It’s usually reversible with good oral hygiene and professional dental care. However, if not addressed, gingivitis can advance to periodontitis. In this next stage, the inner layer of the gum and bone pull away from the teeth to form pockets, which can become infected by bacteria. As the disease progresses, these pockets deepen, more gum tissue and bone are destroyed, and teeth can become loose and may eventually need to be removed.
Debunking Myths and Misunderstandings
Contrary to common belief, gum disease is not always marked by pain or discomfort, and bleeding gums can cease even when the disease persists. It’s a misconception that once bleeding stops, gum disease is cured. Another widespread myth is that gum disease is a rare condition that can be completely avoided with good oral hygiene. While oral hygiene is crucial, factors like genetics, smoking, and systemic diseases such as diabetes can influence an individual’s susceptibility to gum disease.
Treating gum disease often requires a multifaceted approach, including professional cleanings to remove plaque and tartar, medication, and possibly surgery for more advanced cases. Good oral care at home is essential to prevent the onset or progression of gum disease, but professional evaluations are necessary to manage and treat the condition effectively.
The Misleading Sign of Bleeding Gums
Bleeding gums are often one of the first noticeable signs of gum disease, but their absence doesn’t always signal a return to perfect oral health. There are several reasons why gums might stop bleeding, ranging from improved dental hygiene practices to the natural progression of gum disease to more advanced, less inflamed stages.
Why Bleeding May Cease
An individual’s gums may stop bleeding due to rigorous oral hygiene, such as regular brushing and flossing, which reduces inflammation and plaque buildup. It can also be due to the body’s response to ongoing inflammation, leading to a receding gum line where the tissue becomes less prone to bleeding. However, this recession doesn’t mean the disease is gone; it can indicate that the condition has worsened, causing the gum to pull away from the tooth.
Symptom Relief vs. Disease Resolution
It’s crucial to distinguish between the disappearance of a symptom and the cure of an ailment. The cessation of bleeding is merely symptom relief. True disease resolution requires addressing the underlying causes of gum disease, which include bacterial infection and tartar buildup below the gum line. Without professional treatment, these issues can continue to cause damage to the supporting structures of the teeth, even in the absence of bleeding.
Continued vigilance and dental care are essential, as the cessation of bleeding gums might give a false sense of security. Regular dental check-ups and cleanings are imperative for anyone who has experienced gum disease, regardless of whether their symptoms seem to have improved.
Beyond Bleeding: Other Symptoms of Gum Disease
While bleeding is a tell-tale sign, gum disease doesn’t end its announcements there. Various other symptoms can indicate the presence of gum disease, some of which might be more subtle yet equally significant. Understanding these can be pivotal in seeking timely dental intervention and preventing the progression of the disease.
Other Warning Signs
Apart from bleeding, one should be on the lookout for persistent bad breath or a bad taste in the mouth that doesn’t go away, which can be caused by the accumulation of bacteria. Gums might appear red or swollen, and you could experience tenderness or discomfort. Receding gums, which make your teeth look longer, is a sign of advancing gum disease and can lead to sensitivity due to exposed roots. Furthermore, teeth may become loose or separate due to the weakening of the supporting structures, and changes in the way your teeth fit together when you bite can occur.
The Subtlety of Symptoms
Many of these symptoms are insidious. They develop gradually and can be easy to overlook. A person might adjust to the discomfort or the subtle changes in their bite without realizing they signify a serious underlying condition. It’s also common for gum disease to progress painlessly, without any discomfort at all, making regular dental check-ups an essential part of oral health care.
Diagnosing Gum Disease: The Role of Dental Professionals
Gum disease can be a silent affliction, but dental professionals are trained to uncover its subtle signs and halt its progress. A periodontist, a dentist specialized in the treatment of gum disease, plays a pivotal role in the diagnosis and management of this condition.
Expert Evaluation
The initial step in diagnosing gum disease is a comprehensive oral evaluation. During this exam, the periodontist will review the patient’s medical history since systemic health issues like diabetes can influence gum health. The dentist will then perform a visual examination of the mouth, looking for the telltale signs of gum disease such as redness, swelling, and plaque accumulation.
Advanced Diagnostic Tools
Periodontists use advanced tools and techniques to assess gum health thoroughly. A periodontal probe, a small dental instrument, is used to measure the depth of the pockets between the teeth and gums; deeper pockets can indicate the presence of gum disease. Dental x-rays are employed to observe the bone level around the teeth, looking for any signs of bone loss. In some cases, more specialized tests might be used, such as bacterial tests to determine the types of bacteria present, or genetic susceptibility tests.
Treatment and Management of Gum Disease: Navigating Your Options
When it comes to treating gum disease, understanding the array of options available is crucial. It’s not a condition that should be left to self-resolve, especially if symptoms appear to diminish. Let’s explore the treatments and why professional care remains indispensable.
Comprehensive Treatment Options
Treatment for gum disease ranges from nonsurgical therapies that control bacterial growth to surgery to restore supportive tissues. A personalized approach may include:
- Deep Cleaning Procedures: Scaling and root planing are deep-cleaning methods that remove tartar and bacteria from tooth surfaces and beneath the gums.
- Medications: Antimicrobial mouth rinses, antibiotic gels, and oral antibiotics can be prescribed to manage infection.
- Flap Surgery: For advanced disease, a periodontist might perform flap surgery to remove tartar deposits in deep pockets or to reduce the pocket to make cleaning easier.
- Grafts and Regenerative Procedures: When bone and gum tissue have been destroyed, grafts can help regenerate lost tissue and bone.
Ongoing Management and Care
Effective management of gum disease involves regular periodontal care and strict oral hygiene practices. Continuity of care is imperative, even when symptoms such as bleeding gums have ceased, to ensure the disease does not advance unnoticed.
What to Expect During a Dental Visit for Gum Disease
Visiting a dental office for gum disease is a proactive step towards maintaining oral health. Here’s what typically happens during such a visit, particularly when you’re seeing a highly-ranked periodontist like Canal Calem Periodontics – a testament to exemplary care.
Your Periodontist Appointment
Upon arriving, you’ll:
- Discuss Symptoms: Be prepared to discuss your gum health and any symptoms you’ve noticed.
- Oral Examination: The periodontist will thoroughly examine your gums for signs of inflammation, pocket depth, and any recession.
- X-rays: If necessary, X-rays may be taken to check the bone level around your teeth and to identify any potential bone loss.
- Treatment Plan: Based on the findings, a customized treatment plan will be outlined. This could range from deep cleaning to more advanced procedures, if necessary.
A visit to top-ranked periodontists Canal Calem Periodontics means you can expect a combination of advanced technology, expert care, and a thorough approach to diagnosis and treatment planning.
The Role of Home Care in Managing Gum Disease
Professional treatment is half the battle. The other half is what happens at home. Here’s how you can manage gum disease daily:
- Effective Brushing: Use a soft-bristle toothbrush and fluoride toothpaste to gently clean your teeth.
- Flossing: Daily flossing is essential to remove plaque between teeth.
- Antimicrobial Mouthwash: Use as recommended by your periodontist to help reduce bacteria in the mouth.
- Diet: Maintain a balanced diet and reduce sugar intake to decrease the risk of plaque buildup.
- Regular Check-ups: Follow up with your periodontist to monitor your gum health and modify treatments as needed.
When to Seek Professional Help?
Gum disease is a sneaky adversary; it can progress quietly. That’s why understanding when to seek professional help is crucial for your oral health. Here are signs indicating it’s time to visit a periodontist:
- Persistent Bad Breath: If bad breath doesn’t go away with proper oral hygiene, it may signal gum disease.
- Loose Teeth or Widening Gaps: Changes in how your teeth fit together when biting or spaces appearing between them could be a red flag.
- Receding Gums: If your teeth are looking longer than usual, it might be due to your gums pulling back.
- Pain or Discomfort: Any persistent pain in your mouth should be evaluated.
- Bleeding During Oral Care: If your gums bleed when brushing or flossing, don’t ignore it.
Do not wait for these symptoms to worsen. Early intervention can mean a world of difference in treatment and recovery. Read more about how to manage your oral health from home.
Conclusion
We’ve discussed the illusive nature of gum disease and how the cessation of bleeding gums does not guarantee the disease is gone. Continuous, vigilant care is crucial. Even in the absence of overt symptoms, underlying issues could be silently progressing. Therefore, the value of a professional evaluation cannot be overstressed.
Call-to-Action
Concerned about your gum health? Waiting can only exacerbate potential issues. We invite you to take proactive steps for your oral wellness. Schedule your comprehensive periodontal evaluation with Canal Calem Periodontics today. Secure your oral health with expert care.
Disclaimer:
Please note: This blog post is for educational purposes only and does not substitute for professional dental advice. Only a dental professional can diagnose and recommend treatment for gum disease.
Talk to Us About an Appointment